
Scientific Nobility With Journey to Excellence: Amreen Khan #LINO23
Amreen Khan, a biomedical researcher at the Indian Institute of Technology in Bombay and #LINO23 participant,,is working on innovative materials to improve cancer treatment and wound healing. Learn more about her career and her #LINO23 experiences.
New Drug for Cancer Treatment on Track
Lindau Alumnus Perparim Limani is integral part of a team that is developing a new approach to treat cancer.

Cancer and Infections
The connection between cancer and viruses, bacteria and parasites was discussed in two Agora Talks during #LINO70.

The Nobel Prizes in Physiology or Medicine 2019 and 2020
Three of the Nobel Laureates in Physiology or Medicine from the years 2019 and 2020 entered the Lindau stage for the first time.
Nobel Prize in Physiology or Medicine 2019: What Cells Do When the Air Gets Thin
This year’s Nobel Prize in Medicine or Physiology honours discoveries concerning how cells sense and respond to low oxygen levels. The findings illuminate a fundamental aspect of normal cellular metabolism and have important implications for understanding – and perhaps treating – cancer.
Nobel Prize in Physiology or Medicine 2018 – Unleashing the Body’s Dogs of War in the Fight Against Cancer
This year’s Nobel Prize in Physiology or Medicine was awarded to James P. Allison and Tasuku Honjo for their breakthroughs in cancer research.

Tackling the Silent Crisis in Cancer Care
Radiotherapy and imaging are vital in cancer care, but there is large inequality in access between low-middle and high-income countries. New technologies may improve the situation.
CRISPR-Cas: The Holy Grail Within Pandora’s Box
Few molecular techniques have had such an impact on the scientific community and the public alike as the CRISPR-Cas gene-editing tool. What future diagnostic and medical potential does the tool hold?
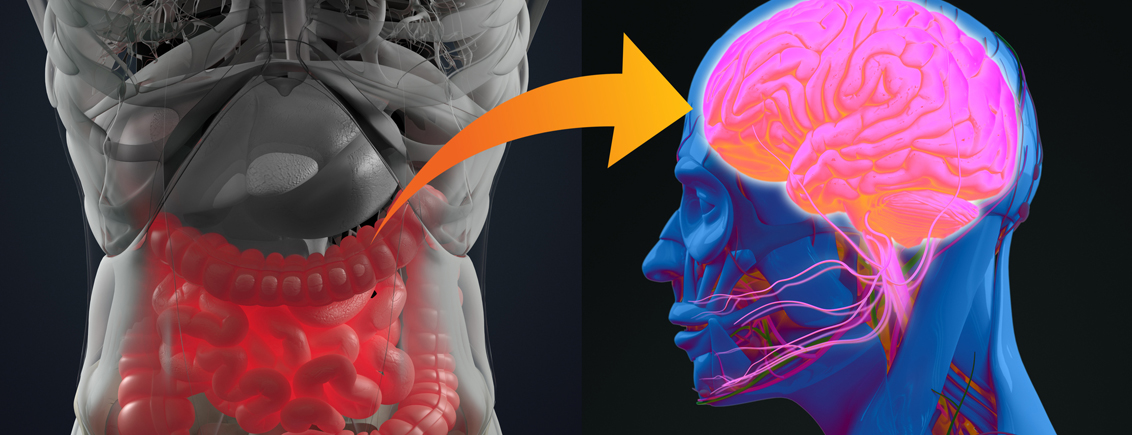
The Hungry Brain
What connects Alzheimer's disease, Parkinson's disease, certain kinds of cancer and obesity? According to several recent studies, the microbiome as part of the gut-brain axis connects all of them and plays a pivotal role when it comes to disease etiology and treatment responsiveness. What connects Alzheimer's disease, Parkinson's disease, certain kinds of cancer and obesity? According to several recent studies, the microbiome as part of the gut-brain axis connects all of them and plays a pivotal role when it comes to disease etiology and treatment responsiveness.
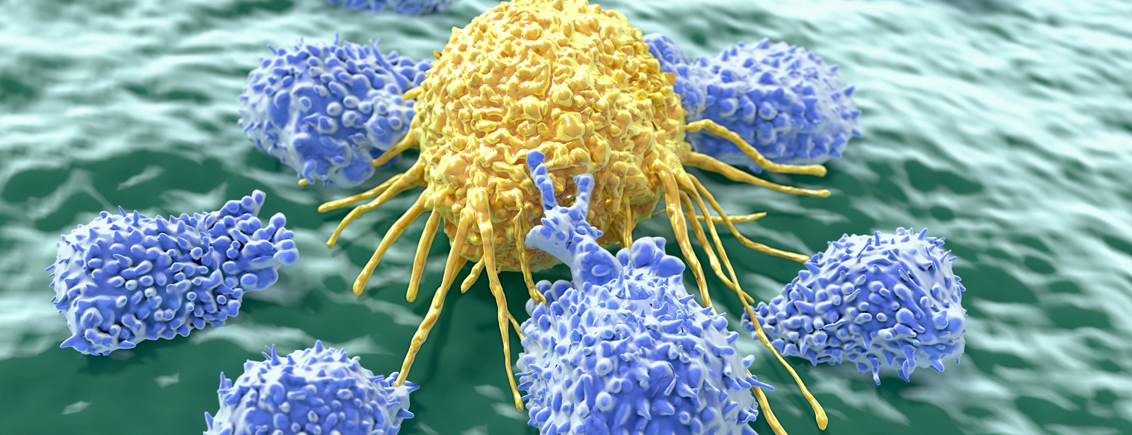
Immunotherapy: The Next Revolution in Cancer Treatment
In some cancer patients, harnessing their immune system to kill tumour cells can lead to long-term remission, but cancer immunotherapy still faces many challenges. In some cancer patients, harnessing their immune system to kill tumour cells can lead to long-term remission, but cancer immunotherapy still faces many challenges.

Digging for the Roots: Cancer Stem Cells
Read about cancer stem cells and their role in cancer research between hype and hopeRead about cancer stem cells and their role in cancer research between hype and hope
Nature film from Lindau chronicles the war against cancer
Rewatch this episode of Nature Video’s Lindau Collection 2014 featuring Lorna Stewart following the past, present and future of cancer research.










